Male Incontinence Specialist

Are you experiencing an accidental leakage of urine or bladder control issues? If so, you may have urinary incontinence. Urinary incontinence can occur at any age and is more commonly seen in older men. Male incontinence specialist, Dr. Mark Allen provides diagnosis and both surgical and nonsurgical treatment options for patients in Plano who are experiencing incontinence.
Contact Dr. Allen’s team today!
An Overview of Male Incontinence
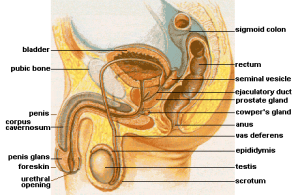
Male urinary incontinence is an accidental leakage of urine. Urine is made by the kidneys and stored in the bladder. A tube called the urethra leads from the bladder through the prostate and penis to exit the body. Around the urethra is a ring of muscles called the urinary sphincter. As the bladder fills with urine, nerve signals tell the sphincter to squeeze shut while the bladder stays relaxed. When males in the Plano, Frisco and Dallas, Texas area suffer from male incontinence, they are encouraged to contact Dr. Mark Allen to learn more about bladder control treatment options.
Reasons for Male Urinary Incontinence
- If the bladder squeezes too hard, or if it squeezes at the wrong time
- If the sphincter muscles get damaged or weak
- If your bladder does not fully empty
- If something is blocking the urethra
Male incontinence happens more frequently in older men than younger men. Urinary incontinence can be chronic or short-term. Typically, short-term incontinence is caused by other health problems or treatments.
Types of Male Incontinence
There are four different types of chronic male incontinence:
- Stress incontinence is the unintentional loss of urine due to physical stress such as coughing, sneezing, running, or heavy lifting. Stress incontinence is rare in men and typically occurs as a post-surgical complication following a prostatectomy.
- Urge incontinence is the involuntary loss of urine when a person has a strong, sudden need to urinate. This condition is caused when the muscles of the bladder contract with greater force than the center muscles of the urethra.
- Overflow incontinence is the urge to urinate, but the bladder does not fully empty. This causes urine to leak later.
- Total incontinence means that there is constant urine leaking. In this case, the sphincter muscle no longer works.
Male incontinence can be an embarrassing issue, which leads men to become reluctant to talk about or seek treatment for this issue. However, once you speak with a urologist you will find there are a variety of treatments available depending on the type of male incontinence you are experiencing, how it is affecting your life, and how aggressive you would like to be about the issue. Most men don’t require surgery to treat their symptoms and have found success with use of medicine, specific exercises, or other specific treatment plans designed by their doctor.
Diagnosis of Male Incontinence
First, a medical history will be recorded, including:
- Major illnesses and surgeries
- Details about your incontinence
- How much fluid you drink in a day and the use of alcohol or caffeine in your diet
- Medicines you take, both prescription and nonprescription
Dr. Allen may ask you to complete a voiding diary, which is a record of fluid intake, trips to the bathroom and any episodes of leakage throughout the day. The void diary helps gain a better understanding of your incontinence and helps direct additional testing.
A physical exam will be conducted to check for prostate enlargement and nerve damage. A digital rectal exam is used to check for prostate enlargement. This exam involves a gloved finger inserted into the rectum to feel for general size and conditions of the glands. To check for nerve damage, Dr. Allen will ask about tingling sensations or feelings of numbness and also check for changes in sensation, muscle tone and reflexes.
An ultrasound, or sonography, is used to obtain images of the bladder and kidneys. Typically, this is completed after you urinate to ensure the bladder has been completely emptied. A transrectal ultrasound may be used to examine the prostate.
Bladder Control Treatment Options
When non-surgical treatment options do not help improve symptoms surgical intervention may be recommended. Dr. Allen will discuss all bladder control treatment options to help decide what treatment will be best for you.
Artificial Urinary Sphincter
An artificial urinary sphincter is a device made of silicone rubber that is used to treat male urinary incontinence. An artificial sphincter is the only device that closely simulates the function of a biological urinary sphincter.
An artificial urinary sphincter is recommended for patients who have urinary incontinence due to the removal of the prostate, sever continual leakage of urine from the urethra and persistent incontinence even after failed treatments.
An artificial sphincter has an inflatable cuff that fits around the urethra close to the point where it joins to the bladder. A balloon regulates the pressure of the cuff and a bulb controls the inflation and deflation of the cuff. The balloon is surgically placed within the pelvic area and the control pump is placed in the scrotum.
To keep urine from leaking the cuff must be inflated. When urination is desired, the cuff is deflated allowing urine to drain out.
This procedure involves abdominal surgery, which will requires hospitalization. Most patients leave the hospital the day after the surgery. While risk is minimal it is important to note some possible complications involved with this procedure:
- Infection of the artificial sphincter
- Wearing away (erosion) of the skin or the urethra
- The artificial sphincter failing to work
90 out of 100 men have successfully treated urinary incontinence with an artificial urinary sphincter.
Sling Procedure
The male sling procedure was developed to treat male urinary incontinence due to sphincter weakness or insufficiencies. This procedure is typically recommended for men with mild-to-moderate urinary incontinence (2 to 3 pads per day or less).
Prior to surgery Dr. Allen may ask you to have a urodynamic study to assess urinary tract function, a 24-hour pad test to identify the number of pads used and the volume of urine leaked, or a cystoscopy to look inside your bladder.
The sling procedure is typically performed as an outpatient, with a fairly short recovery time. The procedure only requires small incisions in the groin. Synthetic mesh-like surgical tape is positioned around part of the urethral bulb, slightly compressing the urethra and gently moving it into a new position. The sling support or suspension requires permanent sutures in the perineum and may create some pain in the immediate post-operative period.
There are minimal complications for this type of procedure. In very rare cases bleeding and infections, erosion, inability to urinate, or recurrent leakage may occur. The sling procedure has been shown to cure many patients suffering from urinary incontinence and others have had significant improvements in their amount of leakage.
For additional information on male incontinence, or to discuss bladder control treatment options, please contact the office of Dr. Mark Allen, urology specialist serving the communities of Plano, Frisco and Dallas, Texas.